Body of Knowledge
Inside the CVS Caremark Interdisciplinary Health Delivery Laboratory at the University of Rhode Island’s College of Pharmacy, teaching and learning tools virtually come to life. They breathe, they blink, they have heartbeats, some even bleed. They can be intubated or given medication, and if treatment goes wrong, they can flat-line. But are they human? No.
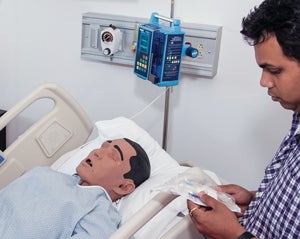 They’re called human patient simulators, or sims for short: mannequins designed with anatomically correct features, realistic skin-feel, and the ability to deliver high-quality and accurate reactions to a variety of medical situations and emergencies. Inside the 3,025-square foot simulation lab, four adult sims, two child-sized sims, and one baby are opening up a world of educational possibilities.
They’re called human patient simulators, or sims for short: mannequins designed with anatomically correct features, realistic skin-feel, and the ability to deliver high-quality and accurate reactions to a variety of medical situations and emergencies. Inside the 3,025-square foot simulation lab, four adult sims, two child-sized sims, and one baby are opening up a world of educational possibilities.
“Many incoming students have the thought that when they graduate, they’ll be going to a local pharmacy and dispensing prescriptions,” says clinical instructor of pharmacy practice and co-director of the lab Amanda DeAngelis-Chichester. “As pharmacists are starting to collaborate with medical teams in hospitals and elsewhere, it’s becoming more and more important for students to see how these medications work in a clinical setting. The sims really crystallize a real-world experience.”
“By the end of the simulation portion of the curriculum, students should be able to run their own patient case,” says professor and co-director of the lab Clinton Chichester III. “We know that this way of learning leads to better retention of knowledge, and more developed skills. We know that we just need to keep moving forward.”
The first sim came to URI 15 years ago, thanks to a generous grant from the Champlin Foundations. Now, the College of Pharmacy and College of Nursing collaborate on the Joint Simulation Program, which allows both colleges to get funding for simulators, with half going to nursing and half going to pharmacy. The lab is used by other disciplines and groups at URI as well, such as communicative disorders, emergency medical technicians, and film students.
 Home
Home Browse
Browse Close
Close Events
Events Maps
Maps Email
Email Brightspace
Brightspace eCampus
eCampus


